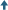But this house, like the one before it, was making him sick with flulike symptoms — nausea, headaches and muscle stiffness.
Lying on the table and breathing in fresh air, Killingsworth thought back to the morning seven years ago when his office was sprayed with Dursban, a potent organophosphate pesticide that has been banned for indoor use since 2000. Within minutes of the pesticide treatment, he was unable to concentrate, and he felt like he had a bad flu. When he returned to the office a week later, he felt sick again. He asked his supervisor to move him to a different office.
“I thought that was the end of it,” he recalls. “But that was the beginning of it.”
Instead of recovering, he got sicker as each year passed. Newly renovated buildings, fresh paint, gasoline odors, pesticides, herbicides — the list of substances he reacted to grew longer and longer. After his apartment was painted by mistake one day while he was at work, he got so ill that he took a leave of absence and moved.
But each subsequent home left him with the familiar panoply of headaches, flulike symptoms, insomnia, the inability to concentrate and fatigue. After sleeping on his dining table for a week, he bought a camping cot and slept on it each night for years. When he became reactive to the almost imperceptible outgassing of chemicals from his own computer, he switched to a Bluetooth keyboard and looked at his computer monitor through the porch window.
Before he got ill, Killingsworth had a girlfriend and an active social life. As his unusual illness escalated, he began to live like a hermit. During his final two years in Georgia, he had fewer than 10 visitors, he says.
Finally, in fall 2007, nine years after his run-in with Dursban, Killingsworth applied for Social Security disability, packed his belongings, and drove west in his Honda Civic to search for housing among a community of folks like himself — all suffering from what is loosely called “environmental illness” — in the remote high desert of Arizona.
Today, in his 40s, he lives in a renovated travel trailer specially designed for his sensitivities: It has porcelain tile floors, sealed walls and sealed wood cabinetry. He camps alone and with friends. He relies on solar power, hauls his own water at times and moves seasonally to avoid extremes of heat and cold. Most days, however, he can tolerate the trailer only for a while, even with windows open, and sleeps on a cot in the back of his truck, under the protective camper shell.
A Two-Step Process
If anybody can understand what happened to Killingsworth, it is physician Claudia Miller, an environmental health expert at the University of Texas School of Medicine in San Antonio, who studies a phenomenon she calls toxicant-induced loss of tolerance (TILT). The word toxicant refers to a man-made poison, such as Dursban, whereas a toxin is a naturally occurring poison produced by living cells or organisms, such as spider venom.
TILT, says Miller, is a two-step process: First, a susceptible individual gets sick after toxic exposure or exposures. But then, instead of recovering, the neurological and immune systems remain damaged, and the individual fails to get well. The sufferer begins to lose tolerance to a wide range of chemicals common in everyday life.
The latest research, both in the United States and abroad, suggests that brain processing itself is altered so that the neurological setpoint for sensitivity falls. The person, now sick, becomes highly sensitive to chemical exposures. The individual is like a fireplace after the original fire has died down: The embers still glow a brilliant orange, ready to burst into flame with the slightest assistance.
Individuals with TILT can become increasingly more reactive over time, until they find themselves responding adversely to the mere whiff or dollop of everyday chemicals — at concentrations far below established toxicity. The triggering substances are often structurally unrelated and range from airborne molecules to ordinary drugs and supplements, lotions, detergents, soaps, newsprint and once-cherished foods like chocolate, pizza or beer.
Exposures result in a bewildering variety of symptoms such as cardiac and neurological abnormalities, headaches, bladder disturbances, asthma, depression, anxiety, gut problems, impaired cognitive ability and sleep disorders.
Because so many substances seem to spike these overlapping reactions, and because not everybody is universally reactive to exactly the same substances, it’s hard to ferret out cause and effect. And that has, until recently, left these individuals consulting many different specialists, presenting a picture that looks deeply neurotic.
When chemically intolerant patients first came to the attention of the medical profession in the 1980s, their condition was called “multiple chemical sensitivity” (MCS), and there was enough curiosity to spark studies. But those studies never turned up anything definitive, and nobody thought to look at the actual processing going on in the brain.
They would test patients by exposing them to odors in a “blinded” situation, where they did not know what they were being exposed to, or they were told harmful odors were present when there were no odors at all. The patients often failed to demonstrate any consistent response.
Studies on detoxification pathways — the immune mechanisms by which the body dismantles toxins — were few and far between; research never explained how certain exposures could snowball into the profound dysfunction reported by this hobbled patient group. Immunological abnormalities were investigated, but not one was ever consistently tied to the condition overall.
So for decades, these patients were cast aside as mentally ill. If you see a person wearing a honeycomb mask in the detergent aisle of the supermarket, if they tell you that the fabric softener scent you love is making them ill, if they say your perfume is causing headaches and asthma and that the carpet store causes brain fog, irritability and depression, your reflexive response may just be, “You may be sick, but you are probably sick in the head.”
Science for Toxic Times
For scientists studying the illness, however, that view has changed, in large part due to Miller’s indefatigable research and her groundbreaking finds. According to a July 2012 study of 400 primary care patients (published by Miller and her colleagues in the popular family practice journal Annals of Family Medicine), 22 percent of individuals with chronic health issues suffer from some degree of chemical intolerance. That’s more than one in five — and, says Miller, they are vulnerable to TILT if life happens to toss them too much toxic exposure.
“The fact that chemical intolerance is so prevalent, yet unrecognized, is important for primary care physicians,” says physician David Katerndahl, Miller’s colleague and lead author on the study. “On the one hand, simple therapeutic approaches (avoiding chemicals) may be quite effective, while on the other hand, conventional treatments (allergy shots, immune suppressants) may fail. This means that we must change our clinical paradigm with these patients.”
The new study is based on an inventory of 50 questions called the QEESI (the Quick Environmental Exposure and Sensitivity Inventory, available for free at familymed.uthscsa.edu/qeesi.pdf). The QEESI isolates sensitivities to common triggers, such as diesel, paint thinner, foods and products like fabric softener. It is very effective at culling the one in five individuals who are vulnerable to severe TILT, and it has been validated in Sweden, Denmark, Japan and the United States.
It is severe TILT, where the individual’s life is seriously impacted, that worries Miller, however. “In the study, I was astounded to find that over 6 percent of people visiting a primary care clinic for any kind of chronic health condition were greatly affected by TILT, based on their symptoms and chemical and other intolerance scores from the QEESI. By greatly affected, I mean that they had chronic health symptoms that were severe, and they scored high on sensitivities to common chemicals, foods and medications,” says Miller. “Another 15.8 percent were moderately affected, with scores that were still well above average.”
Miller’s mission is to catch those vulnerable folks, like fish in a net, before they run headlong into a toxic exposure that derails their lives. She would like to see the QEESI given as standard practice along with the typical sheaf of forms patients fill out.
“TILT describes a genuinely new class of diseases unique to our toxic, modern times,” says Miller. “People suddenly cannot tolerate chemicals and exposures they’d tolerated their whole lives. It’s the hallmark of TILT. Some people I’ve counseled even use it as a verb. They say they’ve been ‘tilted.’”
Navigating a Tilted World
The two-step process of TILT — getting sick upon toxicant exposure and failing to get well — may be driven by epigenetic changes, which occur when the environment alters the expression of genes without changing the core DNA code itself. “Environmental events can dramatically impact gene activity,” explains reproductive endocrinologist Frederick vom Saal of the University of Missouri-Columbia.
Vom Saal has spent several decades researching the potent effects of everyday low-dose exposure to chemicals like bisphenol A (BPA) that are known as endocrine disrupters. These chemicals act like hormones and have profound influences on health, particularly during fetal development. It turns out that surprisingly low doses can be potent regulators of gene activity, while high doses simply shut activity down.
“Once genes are switched on,” says vom Saal, “and once you are sensitized, you essentially have a reprogrammed cell. And it’s hard for that cell to go back to its original state. You will find, for instance, that mammary tissue is more vulnerable to cancer later in life, or puberty occurs earlier than normal because of low-dose exposures in the womb. Although I personally study epigenetics during development, evidence suggests these kind of events occur throughout life.”
In the world of TILT, dose does not make the poison. Dose plus host makes the poison — and host susceptibility is the missing link. In the genetically vulnerable, too much toxic exposure seems to recalibrate the body for life. “All changed, changed utterly,” as poet William Yeats might say; a new person emerges, for whom the ordinary world is now littered with seemingly toxic land mines, often not perceived until stumbled upon, and yet the sufferer looks on as others blithely dance over those same land mines without the hint of a problem.
To Miller, the kind of pesticide poisoning Killingsworth suffered is a truly elegant, if terrifying, example of TILT. In the mid-1990s, she and her colleague Howard Mitzel surveyed 37 individuals who had become permanently ill after an exposure to organophosphate pesticides, and another 75 individuals who got ill after extensive remodeling in the home or office.
In both cases, exposure to toxic substances left a permanent damaging footprint, though pesticide sufferers were by far the sicker group. At the time of their pesticide exposure, 26 of the 37 pesticide individuals were working full time. By the time of the survey (an average of about eight years after exposure), only two of the pesticide individuals were able to work full time. They reported that their illness had affected every aspect of their lives.
TILT looks much the same across cultures and countries. Miller co-authored a textbook, Chemical Exposures: Low Levels and High Stakes, with MIT policy and technology professor emeritus Nicholas Ashford. In that book, Ashford reported on his research in nine different European countries, and he found the same patterns of inexplicable new-onset intolerance to chemicals.
“I simply asked physicians if they’d ever had patients who developed unusual and inexplicable responses to anything that had never bothered them before,” he says, “and I inevitably got a nod yes, and stories.” Miller, meanwhile, has documented similar reports from the United States, Canada, Japan, New Zealand, Great Britain and Australia.
New-onset intolerances and multisystem symptoms have shown up in sheep dippers in rural areas of Europe (sheep dip is an organophosphate pesticide), homeowners in Germany exposed to a toxic wood preservative, individuals breathing fumes from massive oil spills, radiology workers in New Zealand who inhaled chemicals while developing films, and individuals living or working in newly remodeled buildings.
In 1987, 225 workers renovating the EPA’s headquarters in Washington, D.C., got sick after extensive remodeling of a poorly ventilated office building that included the installation of 27,000 feet of new carpet. Although most recovered, 19 developed TILT and became so disabled over the long term that they sued the building owners.
Gulf War veterans were another “tilted” group. Their illness was long the subject of controversy, and even dismissed as a form of post-traumatic stress disorder, but it has recently been accepted as genuine. Miller found that a surprising number of Gulf War veterans turned out to suffer from TILT.
“Of 700,000 who went to war in 1990, 250,000 came back with chronic illness,” she says. “A CDC study found that sick Gulf War veterans reported more chemical intolerances than their healthy counterparts. They had multiple toxic exposures, including pesticides in their tents, smoke from oil fires, anti-nerve-gas pills and diesel fuel poured on the ground to keep the sand down.”
When Miller visited veterans, some had signs on their room doors: “Don’t enter if you’re wearing fragrance.” Many were having trouble tolerating medications. One veteran had sent his wife a favorite perfume from overseas, but when she wore it on their car ride home, he became so sick he asked her never to wear it again. They’d report they felt better on a vacation in, say, the high mesas of Colorado, and spaced out and sick driving in heavy traffic.










![pwanniemedium[1]](http://www.purewatergazette.net/blog/wp-content/uploads/2012/05/pwanniemedium1.jpg)
![pwanniemedium[1]](http://www.purewatergazette.net/blog/wp-content/uploads/2012/05/pwanniemedium1-246x300.jpg)